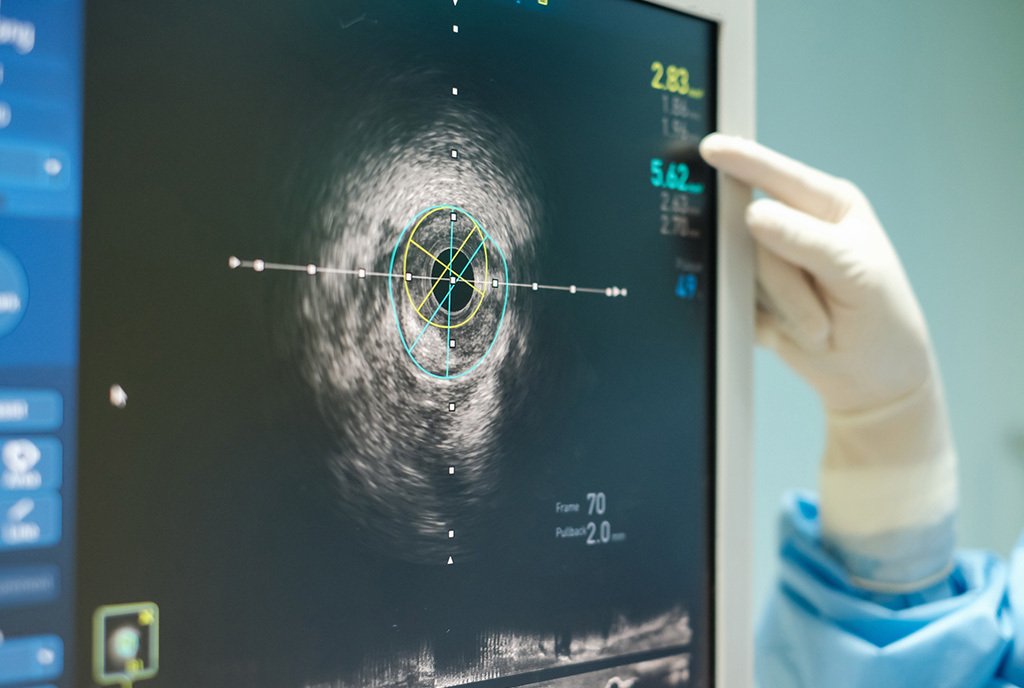
Since 1950, heart disease has been the leading cause of death in the United States, causing heart attacks, strokes, and vascular dementia due to mini-strokes. Despite this—and despite the ease of screening using noninvasive ultrasound technology, especially if pocket ultrasound devices are used—artery screening remains rare.
Due to its utility for detecting potentially dangerous cardiovascular conditions, some people have chosen to pay a private provider for carotid artery screening without reimbursement from their health insurance. Over a six-year period, 3.6 million US adults opted to pay out of pocket for ultrasound artery screening.
Unfortunately, most people go without screening, including people with low socioeconomic status or anyone experiencing financial strain, who—as research has shown—are at increased risk of heart disease and who presumably are not able to pay out of pocket.
To help address this gap in access to artery screening, Congress could provide funding to enable America’s 15,000 community health clinics to offer free artery screening for their patients once they reach a certain age and to repeat the screening at an appropriate interval.
Over a six-year period, 6 million US adults opted to pay out of pocket for ultrasound artery screening.
Community health clinics are funded by the US government to provide medical care to more than 30 million people in areas where economic, geographic, or cultural barriers limit access to healthcare. Of the patients they serve, 80 percent are either uninsured or covered by Medicaid or Medicare, and 90 percent have family incomes at or below 200 percent of the poverty line.
Artery Screening’s Role in Reducing Cardiovascular Risk
Five cardiologists have advocated for artery screening, writing in the Journal of the American College of Cardiology that primary care providers should screen their patients for artery-clogging plaque and offer a prescription for “intensive” statin therapy for those who have plaque in their arteries to prevent heart attacks and strokes.
The most common forms of heart disease are caused by artery clogging, also known as atherosclerosis. The clogging of an artery that serves the heart muscle can lead to a heart attack, while the clogging of an artery that serves the brain can lead to a stroke.
Offering artery screening to patients at community health clinics to detect early-stage heart disease could, for many patients, lead to treatment that adds healthy years to their lives.
Doctors now use a risk-scoring approach to decide when to initiate treatment for heart disease based on factors such as the level of “bad,” low-density lipoprotein (LDL) cholesterol in the blood, and whether the patient smokes or has high blood pressure, diabetes, or a family history of heart disease. Yet one study found that nearly 60 percent of those classified by risk scoring as having low risk for heart disease in fact had early-stage artery clogging, which researchers detected primarily through ultrasound artery testing. The researchers said this finding suggests the “added value of imaging for prevention.”
In an article in the Journal of the American Medical Association, two cardiologists argue that the risk-scoring approach allows artery clogging “to proceed unchecked for decades.”
However, the risk-scoring approach is currently the medical standard, and it’s the approach doctors are trained to use. As a result, few doctors routinely offer artery screening to their patients.
Saving Lives, Saving Money: Making the Case for Preventive Artery Screenings
Offering artery screening to patients at community health clinics to detect early-stage heart disease could, for many patients, lead to treatment that adds healthy years to their lives—all while reducing costs for the US healthcare system.
The argument that artery screenings save lives rests on a simple set of considerations. First, consider that according to the European Atherosclerosis Society Consensus Panel, “bad” LDL cholesterol in the blood causes heart disease. Next, consider that early-stage heart disease has been found even in people with “normal” LDL levels who did not have known risk factors for heart disease, according to a study by 11 researchers in Spain. They found that among healthy middle-aged adults whose LDL level was well below the top of the range considered normal, 19 percent had artery clogging, identified primarily by ultrasound artery screening. At the highest LDL level found in the study group of otherwise healthy adults, the percentage with artery clogging rose to 64 percent.
Sign up for our free newsletters
Subscribe to NPQ's newsletters to have our top stories delivered directly to your inbox.
By signing up, you agree to our privacy policy and terms of use, and to receive messages from NPQ and our partners.
Researchers have reported that for those with early-stage heart disease, treatment with a high-intensity statin medication can slow or stop the progression of artery clogging. Statins reduce the level of LDL in the blood and stabilize existing plaque in the arteries, reducing the likelihood that a plaque will rupture and cause a clot that reduces blood flow. Plaque rupture is the cause of most heart attacks.
Statin drugs are generic and thus inexpensive—and have been found to be generally safe, according to the American College of Cardiology and American Heart Association Task Force on Clinical Practice Guidelines, and a Task Force for Cardiovascular Disease Prevention that included the European Society of Cardiology, the European Association of Preventive Cardiology, and 12 other medical societies.
Detecting heart disease through artery screening and providing treatment before it results in a cardiovascular event can, over time, save the healthcare system money. One indicator of the potential cost savings from artery screening is a study that screened 6,073 older adults for carotid artery disease and other preventable causes of stroke. The resulting treatment was estimated to prevent 30 strokes and to have saved the healthcare system more than $2 million, even though the cost for each screening was over $400.
Extrapolating the results if 40 million Medicare recipients were screened, the study projected cost savings of almost $13 billion. This is a conservative estimate since many providers now offer carotid artery screening tests for around $150.
Beyond community health clinics, primary care medical practices could offer artery screening to patients starting at a certain age, even before insurance companies provide reimbursement, to demonstrate their commitment to patients’ health.
The Role of Congress and the US Preventive Services Task Force
Congressional passage of the 2006 Screening Abdominal Aortic Aneurysms Very Efficiently (SAAAVE) Act, which provides a one-time aneurysm screening for men with a smoking history when they enroll in Medicare, was facilitated by a 2005 guideline from the US Preventive Services Task Force (USPSTF) based on a review of the literature on vascular screening.
The HHS secretary should select experts who uphold the value of screening to prevent advanced heart disease, not just to diagnose advanced heart disease.
Dr. Robert M. Zwolak, who was chair of the National Aneurysm Alliance (NAA) in 2006, said the SAAAVE Act’s passage was largely due to the efforts of the NAA, which he described as a coalition of medical and surgical specialty societies, foundations, and corporate partners “whose single goal was to achieve this AA screening benefit for people at risk.”
Regrettably, the USPSTF did not recommend screening for carotid artery stenosis in its February 2021 final evidence review, even though the task force acknowledged that plaque in the carotid arteries in the neck is “a manifestation of systemic atherosclerotic disease, so identifying this condition may potentially lead to changes in medical management to prevent future cardiovascular events,” such as heart attacks and strokes.
The USPSTF stated that the use of screening “as a cardiovascular disease risk-stratification tool to identify those with elevated 10-year cardiovascular disease risk who are eligible for statin use” was “outside the scope of this review.” The task force guideline instead focused on the value of screening to identify patients with advanced heart disease who need vascular surgery.
Action by Congress now to fund artery screening at community health clinics would be facilitated by endorsing artery screening by the US Preventive Services Task Force.
USPSTF members are appointed by the secretary of the US Department of Health and Human Services (HHS). In making future appointments, the HHS secretary should select experts who uphold the value of screening to prevent advanced heart disease, not just to diagnose advanced heart disease. That would mean considering the perspective of cardiologists who work to stop the progression of heart disease, not simply the perspective of intervention-focused cardiologists who perform surgery to treat advanced heart disease.
With or without a USPSTF endorsement, Congress can take action to help prevent heart attacks, strokes, and vascular dementia among the more than 30 million Americans served by community health clinics. Artery screening provides a sound, upstream approach to healthcare that could save lives and improve people’s quality of life while reducing healthcare costs. The time is ripe for an effort like the NAA’s work to pass the SAAAVE Act, this time directed to the passage of federal legislation that funds artery screening for those served by America’s 15,000 community health clinics.









