March 10, 2020; New York Times
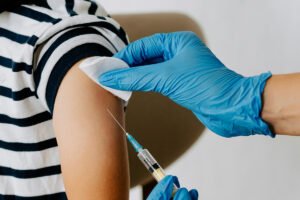
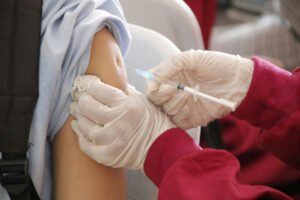
In the midst of a public health crisis, some are more at risk for infection than others, and as the New York Times reported yesterday, there is a perfect storm of conditions in some nonprofits that may lead to tragedy. Bob McElroy, who runs a 300-bed homeless shelter out of a tent in San Diego County, knows this as a fact of life following an outbreak of the normally treatable Hepatitis A three years ago that killed twenty—mostly homeless—people.
It’s not just that the site is so densely packed; many of the residents are over 50 and have compromised health. (One study has indicated that 30 percent of homeless people have chronic lung disease, and COVID-19 is a respiratory illness.) So, while the rest of us are considering whether or not to cancel a conference, and both Yale and Harvard (among a large number of colleges and universities) have sent students off-campus to attend classes online for the time being, congregate living facilities necessitated by poverty, physical abuse, and illness or disability face many more urgent issues with woefully inadequate resources.
It is worth noting that the largest number of deaths associated with a single site was in a nursing home in Seattle. As a result, many residences for older people are restricting visits from those who may have come in contact with someone sick. This kind of precise prevention isn’t really possible in a shelter environment, so what we see instead are things like New York City’s 11-page guidance document “instructing shelters to screen people for symptoms and quickly identify and isolate those who have contracted the virus in a separate room ‘as much as possible.’”
Dr. Helen Chu has been agitating for more testing among Seattle’s homeless population, but she knows full well that even that measure may be a road to nowhere since homeless people have no place to self-quarantine.
Sign up for our free newsletters
Subscribe to NPQ's newsletters to have our top stories delivered directly to your inbox.
By signing up, you agree to our privacy policy and terms of use, and to receive messages from NPQ and our partners.
We should remember at this point that medical debt is a big factor in bankruptcies in this country. One story in this article described the perfect storm in other terms:
In some cases, it was illness that sent many of those living on the street there in the first place. Tracy Semrow, who was a school psychologist earning a six-figure salary working with children with disabilities, learned two years ago that she had a degenerative connective tissue disorder. The costs of medical care have drained her savings.
Since August her home has been one of the bunk beds in the shelter run by Mr. McElroy’s charity, Alpha Project. She is frequently sick and sometimes cannot get out of bed.
“My immune system has gone haywire,” Ms. Semrow said.
Dr. Robert T. Schooley, an infectious disease expert in San Diego, says the virus has transmission rates above 80 percent within households—and, he reminds us, homeless shelters are essentially giant households.—Ruth McCambridge