November 7, 2018; Los Angeles Times and Vox
When the Affordable Care Act was signed into law in 2010, Medicaid expansion was supposed to happen automatically. But in 2012, even as the US Supreme Court upheld the law in National Federation of Independent Businesses v. Sebelius, it also restricted its application, finding, as Adam Liptak wrote in the New York Times, that “Congress had exceeded its constitutional authority by coercing states into participating in the expansion [of Medicaid] by threatening them with the loss of existing federal payments.”
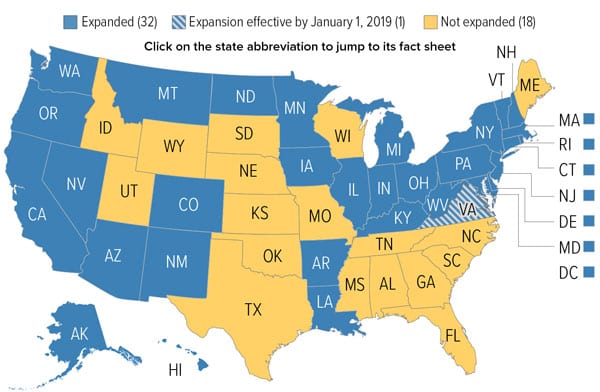
To date, 33 states and the District of Columbia have elected to expand their Medicaid systems to provide greater health insurance coverage. But in the remaining 17 states, approximately 2.2 million lack the healthcare coverage they would have otherwise received. These people fall into the category of “working poor,” earning too much to qualify for traditional Medicaid but too little to be able to afford health insurance on their own. According to a recent report from the Center for American Progress, extending coverage to all of these 2.2 million would save over 14,000 lives a year.
Tuesday’s elections will extend coverage to at least 300,000 of these 2.2 million. In three states where Medicaid expansion was on the ballot, voters made their wishes known. Sarah Kliff summarizes the election returns in Vox:
In Idaho, the Medicaid expansion passed by an especially large margin, with 61 percent in favor and 39 percent against. The Nebraska expansion passed with a tighter margin: 53 percent of voters in favor, and 47 percent against. And in Utah…the vote still hasn’t been certified by the state, but…the proposition leads with 54 percent of the vote.
Sign up for our free newsletters
Subscribe to NPQ's newsletters to have our top stories delivered directly to your inbox.
By signing up, you agree to our privacy policy and terms of use, and to receive messages from NPQ and our partners.
These votes raise the number of states with expanded Medicaid to 36. But other states may join them. In Kansas, and Wisconsin, Republican governors had blocked Medicaid expansion, but with new Democratic governors now elected in those states, the number with expanded Medicaid may rise to 38. On the other hand, in Montana, an initiative to raise tobacco taxes by $2 a pack to make Medicaid expansion permanent (Initiative 185) was defeated by a 53 percent to 47 percent margin. As many as 100,000 may lose coverage in that state.
The stories of those struggling to get by without expanded Medicaid are often heartbreaking. In Idaho, Audrey Dutton of the Idaho Statesman writes:
Jessica Rachels, 37, from Sandpoint, is a full-time caregiver to her daughter, who has a disability. Rachels was just diagnosed in June with bipolar disorder and has already spent hundreds of dollars on treatment. She said she hasn’t had health insurance in 12 years; her family has had to decide between paying their bills and keeping a roof over their head, or getting her health care.
Rachels and an estimated 119,000 other Idaho residents will now gain Medicaid coverage.
Medicaid expansion, of course, also affects nonprofit operations. Earlier this year, when Virginia expanded Medicaid coverage to 400,000, NPQ noted that some nonprofit healthcare clinics were “considering adopting hybrid models to provide free care and accept Medicaid payments.” A 2017 study written by three Northwestern University business school professors and published by the Commonwealth Fund identified even broader impacts for hospitals. According to the report, “Uncompensated care burdens fell sharply in expansion states between 2013 and 2015, from 3.9 percent to 2.3 percent of operating costs.” At the time, the authors argued that if every state expanded Medicaid, hospitals uncompensated care costs would fall by $6.2 billion.—Steve Dubb












