May 14, 2017; Wall Street Journal
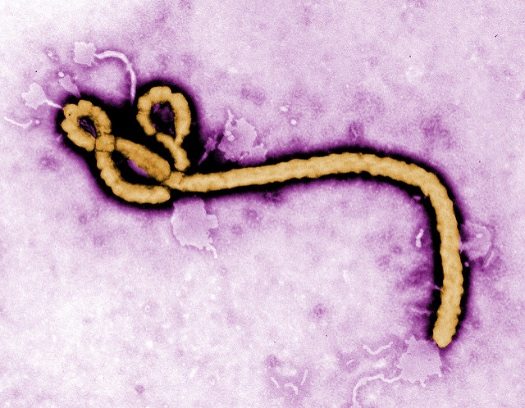
The very word “Ebola” sends waves of dread through many communities. It’s a horrible disease with extremely high infection and mortality rates and no cure. This week, the Democratic Republic of the Congo saw several citizens die of the disease, and the nation is scrambling to contain the outbreak before more are infected.
Unlike Sierra Leone and other countries in western Africa where the 2014 epidemic hit, much of the Congo is densely forested and difficult to traverse. Experts hope that this will slow the spread of the disease. Conversely, as NPQ reported in November, the country has been hovering on the brink of civil war for months, and its health infrastructure has been described by the World Health Organization (WHO) as “virtually broken down.” As Harvard physician Margaret Bordeaux has pointed out, the destruction of institutions and infrastructure kills more civilians in wartime than violence, and the DRC’s violent history has made its civilians perilously vulnerable to even preventable diseases, never mind rampant killers like Ebola.
NPQ tracked the global response to the last Ebola epidemic, which was widely deemed insufficient and, in some cases, unfulfilled. Science journalist Laurie Garrett explained in Foreign Affairs, “The global health infrastructure has shown itself to be weak, fractured, prone to infighting, and more interested in searching for technological silver bullets than engaging in the hard slog of social mobilization and classic local public health work.”
Global disease expert BT Slingsby said,
Ebola was very much a wake-up call for our global society. Regardless of whether we’re dealing with a pandemic, such as Ebola, or antimicrobial resistance, or with more endemic diseases like malaria or tuberculosis—all of those infectious diseases have one thing in common: Innovations do not come from the free market on its own. But we need these innovations—and therapies, vaccines and diagnostics.
Sign up for our free newsletters
Subscribe to NPQ's newsletters to have our top stories delivered directly to your inbox.
By signing up, you agree to our privacy policy and terms of use, and to receive messages from NPQ and our partners.
Some took Slingsby at his word; there is a vaccine for Ebola, though it has not completed the testing and approval process and only appears to work on one of two common strains. The WHO has not yet decided whether to use it in the Congo, but has made preparations just in case.
But while the WHO debates, there are other things that can be done. One of the biggest problems in the last outbreak, apart from insufficient and poorly deployed aid, was the initial failure of health workers to understand the burial traditions of affected communities and how they magnified the spread of the disease. Many cultures have burial rituals that include washing and dressing the body, but in a cruelly ironic twist, Ebola is most contagious right before and after a victim’s death—so anyone trying to bid goodbye to a loved one is especially prone to catch it.
There were also problems of trust: When people died in health facilities, workers who knew safe burial practices often buried bodies in unmarked graves. According to National Geographic, “These disappearances stoked conspiracy theories that Ebola was a hoax. In one, doctors were said to be killing patients to steal their organs. The less people believed that Ebola was real, the less likely they were to bring deathly ill relatives to clinics and to stop honoring their dead relatives in the traditional way.”
And finally, there’s very little incentive for local people to join the SDB (safe and dignified burial) teams because they are often shunned by their communities for doing so. SDB worker Mariatu Karbgo told Irin News, “‘Mamma G’ was the stigma name they gave me in my community, even in my own street. They said ‘I’m a General in dead bodies’… whenever they saw me they’d gather in a group, and shout ‘General in Ebola!’”
These issues will be familiar to anyone who does community work. It’s important to gain the trust of your community, to learn about the complex issues faced by the people who live where you work and how a situation is locally understood. The goal of Ebola containment and prevention is not flexible, but the approach can leverage local resources—like the Freetown officials in Sierra Leone who eventually asked local imams to explain ritual workarounds and convince people that the rules were not absolute, causing a 1,000 percent jump in the number of safe burial teams.
There are many lessons to be applied to the newest Ebola outbreak, and hopefully the scale will remain small. In an already fragile state, it will take enormous effort to create a health infrastructure that could deal with problems like Ebola and the cultural competency to enlist the community. Nonprofits who step in will certainly have their work cut out for them.—Erin Rubin












