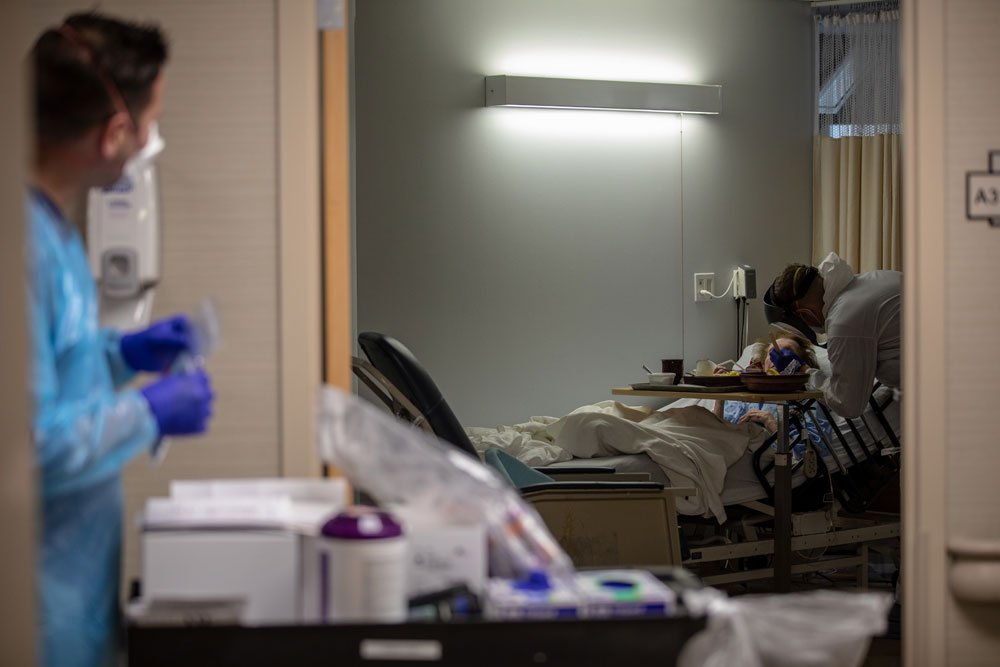
We knew that our nation’s nursing homes and long-term care facilities were inadequate, but few knew it was this bad. As of May 9, 2020, the New York Times reports 25,600 residents and workers had died from COVID-19, about one third of the country’s total deaths related to the coronavirus pandemic. Although there is no doubt that older people are more vulnerable to COVID-19, and congregate living creates a perfect environment for the virus to spread, the reasons for the catastrophe unfolding across the country are more complex.
Advocates for nursing home residents have long been concerned about the quality of care provided in our nation’s skilled nursing facilities. Well before COVID-19, the failures of institutional care were apparent to anyone who visited a home where residents lined the hallways, activities were limited, and staff barely kept up with basic personal care needs. This certainly is not the case everywhere—many exceptional homes provide residents meaningful relationships and experiences that enrich their lives—but the failures of the system overall are on full display as the pandemic rages.
As UC San Francisco professor emeritus Charlene Harrington, who studies nursing homes, tells the Los Angeles Times, “Nursing homes would like the public to think this just happened to them, but it didn’t.” Referring to the large private chains that now dominate the US nursing home sector, Harrington says, “The chains were bad to begin with, and then they were just not prepared for this pandemic.”
Multiple structural issues underlie these failures: ownership; staffing; and payment and oversight. Add to these the failure of the federal government to provide adequate support for testing and access to personal protective equipment (PPE), and the recipe for disaster is complete.
Ownership
A few decades ago, nursing homes were primarily owned and operated by mission-driven nonprofits and small independent, often family-owned, operations. Today, 70 percent of nursing homes have for-profit ownership, many of them held by private equity investors. These investors have found multiple ways to wring profits out of a challenging business that is almost wholly paid for through public dollars—much of it through Medicaid. When profit comes first in a sector that is at-best poorly funded by the government, you don’t get efficiency as investors would tell you. You get declines in quality, including poor infection control.
To profit from a business with razor-thin margins, investors set up real estate trusts to own the buildings, and lease the buildings to operating companies, shielding the investors from liability. In addition, they set up networks of limited liability companies, or LLCs, to sell management services and supplies to the nursing home operator—businesses that are lucrative, even when the nursing home itself is losing money.
“The structure is designed to keep liability on the company that has the fewest assets and the most debt,” William Murray, a lawyer who sues nursing homes on behalf of families, told the New York Times.
A New York Times investigation found that nursing homes owned by private investors “disproportionately lag behind their nonprofit counterparts across a broad array of measures for quality.” Quoting from a recent study of private equity buyouts of nursing homes, the Times reporters wrote, “Private equity owners tended to put ‘high-powered, profit-maximizing incentives’ first.” Sabrina T. Howell, assistant professor of finance at NYU Stern School of Business and one of the report’s authors, attributed the decline in quality to “staffing cuts.”
The Los Angeles Times reported on one such chain, Plum Healthcare, which is the parent company for 13 of the 192 nursing homes in California that have reported outbreaks. Plum accounts for 500 cases of COVID-19 and 43 deaths, yet Plum told the L.A. Times it “doesn’t run skilled nursing facilities.”
“Plum Healthcare doesn’t own any of the facilities but is contracted by the licensed owner of each entity to perform clinical and administrative services,” a spokesperson explained. “In this regard, we support our clients’ effort to implement their clinical care, infection control and safety protocols.”
This is definitely not a recipe for accountability.
Staffing
Noting the relationship between the byzantine ownership structures that dominate nursing homes, staffing, and the spread of the virus, Harrington says, “It’s not an accident that these chains have [the virus], because they are the ones with the lowest staffing and the worst quality.”
The ownership structure at places like Plum Healthcare is a setup for the nursing home operators, many of whom have gone bankrupt and closed homes in recent years. Responsible for providing for the residents, their budgets are squeezed—sometimes due to high rents and demands to buy supplies from the owner’s other companies—making it more difficult to provide adequate staffing, the most important factor in providing high-quality care.
Many nursing homes simply don’t have enough well-trained certified nursing assistants. With the economy humming along before the current crisis, attracting certified nursing assistants became a severe challenge. Average wages in 2018 were $13.38 per hour for work that is physically and emotionally challenging, is poorly supported, and is not valued by society at large. Training is also insufficient, with 20 states requiring only 75 hours, a minimum standard established by the federal government in the 1980s.
Sign up for our free newsletters
Subscribe to NPQ's newsletters to have our top stories delivered directly to your inbox.
By signing up, you agree to our privacy policy and terms of use, and to receive messages from NPQ and our partners.
Because of the poor quality of the jobs, more than half of certified nursing assistants (CNAs) are women of color, a factor that then leads to further disrespect of employees and discrimination. Wages have remained stagnant for a decade or more, resulting in 44 percent of nursing assistants living in households with incomes below 200 percent of the poverty level. This drives nursing assistants to take multiple jobs at different facilities, which has been one of the ways the virus has spread.
Nonetheless, many of the women who do these jobs are deeply committed to the elders they care for. They bring their hearts and souls regardless of the quality of the training, support, and wages. Now they have been left unprotected, without adequate testing so they know who is sick, and without masks and gowns to safely care for residents with COVID-19. Many have died as a result.
“Alice,” a CNA, spoke under a pseudonym with Amy Costello for her podcast, Tiny Spark:
For the longest time, we didn’t have any [personal protective equipment]. But as of last week, they managed to give us a shield, a gown, and a mask. But we have to use this, keep it for about a week. So that means you just you keep using it, reusing it, reusing it…. You’re going from room to room, room to room with the same gown. And it’s so easy to transmit whatever is on the gown to them.
Nursing homes also are required to have registered nurses on staff. In an investigation of the relationship between nursing home quality and the spread of COVID-19 in California nursing homes, Kaiser Health News found that homes that experienced COVID-19 infections had on average 25 percent fewer registered nurses per resident in the last three months of 2019. These nursing homes also had significantly more infection-control violations—not a surprising outcome with inadequate nurse management and supervision.
Payment and Oversight
Regardless of quality, nursing home care is expensive. The average annual cost is $90,000. For six of every ten nursing home residents, Medicaid pays the bill. Although it is difficult to fully assess, the American Health Care Association, the lobby group for for-profit nursing homes, claims that average reimbursement of about $200 per day does not cover the costs of care. That is a poor formula for providing robust training and staffing.
Unable to squeeze more out of Medicaid, the lobbyists for nursing homes have made a full court press to reduce regulation. Under the Trump administration, the Center for Medicare and Medicaid Services (CMS) has reduced staffing requirements and proposed eliminating an Obama regulation that would have required every facility to hire an on-site infection control specialist. These decisions were bad to begin with, but as tens of thousands of older Americans die as a result of inadequate infection control, they appear utterly negligent.
Now nursing home leaders are asking for a $10 billion bailout and immunity from lawsuits related to COVID-19. Fifteen states have already agreed to shield them. If Congress includes the bailout funds in the next version of the CARES Act, the funds should be required to be used to support frontline staff, testing, and acquiring sufficient personal protective equipment.
What Can Be Done?
Cities and states are realizing that they must focus their attention on nursing homes to stem the tide of coronavirus infections. Despite the inadequate response of the federal government, which still has no public system for tracking infections in nursing homes and has still not convened its Coronavirus Commission for Safety and Quality in Nursing Homes, some states and cities are stepping up. Detroit has implemented testing of all nursing home residents, and New York, which has been criticized for not acting quickly enough, is ramping up data collection, testing, and provisions to move residents when homes cannot adequately protect them.
Sunil Parikh, a Yale University physician and public health expert, writing in STAT, offered a list of actions that need to be taken to stop the rising death counts in nursing homes and other long-term care facilities. State leaders should add these immediately to their to-do lists:
- Provide all nursing homes with adequate personal protective equipment for staff.
- Make COVID-19 tests available for testing all residents and staff, especially if a single infection has been reported.
- Support leadership and staff with training in how to reconfigure their facilities to separate infected residents from those who are not infected. (This is extraordinarily difficult in many facilities, so funds to enable homes to access expert advice and technical assistance are needed.)
- Provide infection-control training, and sufficient workforce support to ensure implementation.
- Support workers financially so they don’t need to work in multiple facilities.
Parikh writes, “Preventing new infections [in nursing homes] will limit the needless deaths of thousands of Americans, reduce the demand for person protective equipment, and lower the risks of infection borne by frontline health care workers.”
But we should go further. The coronavirus has revealed the crumbling structure of a wholly inadequate system of care for America’s most vulnerable elders. It’s time to get serious about providing for the health and safety of elders in environments that support good health and quality of life. That requires us to value the work of certified nursing assistants and offer them the training, support, and wages they deserve.
We also must ask ourselves whether for-profit entities belong in this field when profits are too often had at the expense of quality care. Nursing homes may be a field where profitmaking is inappropriate and, indeed, potentially fatal.












